 A newly published study led by Peter Newton, M.D., finds that anterior spinal growth tethering (ASGT) is a viable alternative to spinal fusion for certain patients with thoracic scoliosis. It is the longest follow-up study on spinal tethering patients done to date.
A newly published study led by Peter Newton, M.D., finds that anterior spinal growth tethering (ASGT) is a viable alternative to spinal fusion for certain patients with thoracic scoliosis. It is the longest follow-up study on spinal tethering patients done to date.
ASGT has been shown to alter spinal growth with the potential to correct scoliosis while maintaining spine flexibility. The purpose of this study was to report the two- to four-year outcomes of ASGT in skeletally immature patients with thoracic scoliosis.
The researchers conducted a retrospective review of patients with thoracic scoliosis who underwent ASGT with a minimum of two years of follow-up. Patient demographics, perioperative data and radiographic outcomes are reported. A “successful” clinical outcome was defined as a residual curve of <35° and no posterior spinal fusion indicated or performed at latest follow-up.
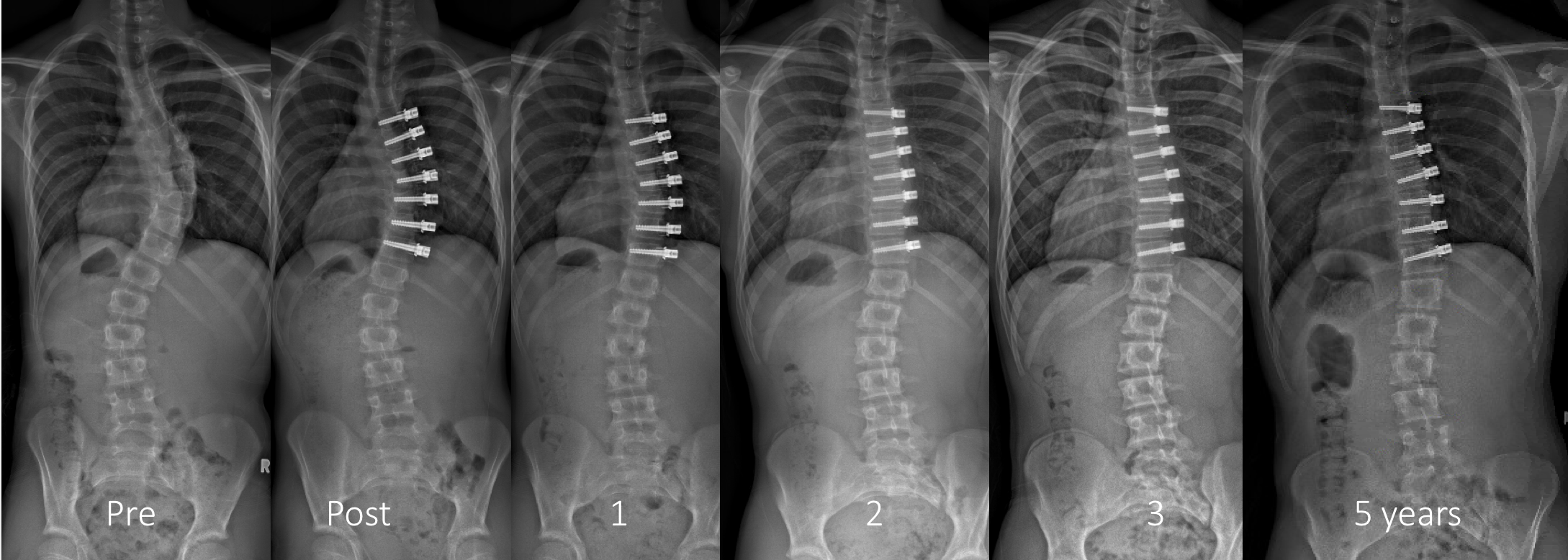
Seventeen patients met the inclusion criteria. The etiology was idiopathic for 14 and syndromic for three. The mean follow-up was 2.5 years (range, 2 to 4 years). Preoperatively, all patients were at Risser stage 0, with a mean age at surgery of 11 ± 2 years (range, 9 to 14 years). There was an average of 6.8 ± 0.5 vertebrae tethered per patient. The average thoracic curve magnitude was 52° ± 10° (range, 40° to 67°) preoperatively, 31° ± 10° immediately postoperatively, 24° ± 17° at 18 months postoperatively, and 27° ± 20° at latest follow-up (51% correction; range, 5% to 118%). Revision surgery was performed in seven patients: four tether removals due to complete correction or overcorrection, one lumbar tether added, one tether replaced due to breakage, and one revised to a posterior spinal fusion. In three additional patients, posterior spinal fusion was indicated due to progression. Eight (47%) of the patients had a suspected broken tether. Ten (59%) of the 17 were considered clinically successful.
Despite most patients having some remaining skeletal growth at the time of review, the results demonstrate that at mid-term follow-up, ASGT showed a powerful, but variable, ability to modulate spinal growth and did so with little perioperative and early postoperative risk. Fusion was avoided for 13 of the 17 patients. The overall success rate was 59%, with a 41% revision rate.
In Dr. Newton’s view, tethering is “reasonable” for the growing patient with a scoliosis beyond 45 degrees. He notes that an attempt to avoid fusion with a growth modulating tether will be less reliable and have a higher revision rate than posterior spinal fusion.
He stresses the need for patients to know the pros and cons of each procedure. “Some will value motion over the absolute correction or the greater chance of revision,” Dr. Newton says. “Others will value the most reliable approach at the expense of a modest loss of motion. Shared decision-making is mandatory.”
Dr. Newton adds that while there is a growing interest in fusion-less surgery, fusions should not be demonized. “Internet and social media sites praising tethering and damning fusions are doing a disservice,” he says. “Patients need to make an informed decision based on unbiased and accurate information. I hope that this paper will shed light on this topic.”
“Anterior Spinal Growth Tethering for Skeletally Immature Patients with Scoliosis: A Retrospective Look Two to Four Years Postoperatively” appears in the October 3, 2018, issue of The Journal of Bone and Joint Surgery.