Melanoma
What Is Melanoma?
Melanoma (mel-eh-NOE-muh) is a type of cancer that begins in a melanocyte (meh-LAN-uh-site), a cell in the top layer of skin (the epidermis). Melanocytes make melanin (MEL-eh-nun), the pigment that gives skin its color.
Melanoma also can develop in other parts of the body, like the eyes, mouth, genitals, and anal area.
What Are the Signs & Symptoms of Melanoma?
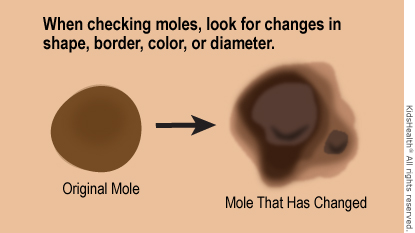
Often, melanoma begins as a mole or a bump on the skin. It’s important to know if a mole has changed in size, shape, or color.
Keep this ABCDE rule in mind when checking moles:
- A for asymmetry: If you were to cut the mole down the middle, would the left and the right sides look different?
- B for border: Are the edges blurry and undefined? Does it look like it’s spreading sideways?
- C for color: Does the mole look darker or lighter than usual, or does it have an area of new color — perhaps black, blue, purple, red, or white?
- D for diameter: Is the mole larger than the eraser on a pencil top?
- E for evolving: Has there been any change in the size, shape, color, or elevation of the mole?
Melanoma most commonly develops on the trunk, head, and neck for boys, and the lower legs for girls.
What Causes Melanoma?
In adults, ultraviolet (UV) light can cause melanoma on any area of skin and can make a mole more likely to turn into melanoma. UV light comes from the sun and from the light in tanning beds. It usually takes many years to develop melanoma from sun exposure.
When a child gets melanoma, sun exposure is usually not the cause. Kids who are born with melanocytic nevi (large black spots) and specific kinds of moles have a risk of melanoma.
Sometimes melanoma begins in an area where there is no dark spot or bump.
Melanoma happens when melanocytes stop working normally. Because of a genetic change (mutation), they begin growing out of control, sticking together to form tumors, crowding out healthy cells, and damaging surrounding tissue.
Who Gets Melanoma?
Risk factors that can increase a person’s chances of melanoma include:
- a fair complexion (light skin that freckles or burns easily)
- blue or green eyes
- blond or red hair
- having many moles (usually, more than 25)
- UV exposure (from the sun or a tanning bed)
- having a history of frequent or severe sunburns
- having a relative with melanoma or a family history of oddly shaped moles
- age (older people are at greater risk)
- having had melanoma before
Though less likely, people can still get melanoma even if they’re young, have no family history of cancer, or have dark skin.
How Is Melanoma Diagnosed?
The doctor will do a biopsy, removing all or part of the lesion (the affected area of skin) and look at its cells under a microscope. A biopsy shows if the cells are cancerous. It can also show how deep they are in the skin, which can help doctors predict the risk of the melanoma spreading.
How Is Melanoma Treated?
Melanoma treatment can include:
- surgery to remove the cancerous lesion
- chemotherapy: tumor-killing medicines are given by mouth, through an injection (a shot), or intravenously (into a vein)
- targeted therapy: specific medicines that find and attack cancer cells without hurting normal cells
- immunotherapy (biologic therapy): when doctors stimulate the body’s own immune system to fight cancer cells
The treatment chosen depends on:
- how big and how deep the lesion is
- what part of the body it is on
- whether the cancer has spread
Can Melanoma Be Cured?
Melanoma that’s caught early, when it’s still on the surface of the skin, can be cured.
Untreated melanoma can grow downward into the skin until it reaches the blood vessels and lymphatic system. This lets it travel to distant organs, like the lungs or the brain. That’s why early detection is so important.
Can Melanoma Be Prevented?
Most childhood types of melanoma can’t be prevented because they are due to a mutation (change in a gene).
The most important way to prevent melanoma from developing later in life is to limit kids’ and teens’ sun exposure.
Keep kids younger than 6 months out of the sun entirely, because their skin is so sensitive. If any skin must be exposed to the sun, use a small amount of sunscreen on those parts, such as the face and hands.
Kids 6 months and older should use sunscreen with an SPF of at least 30 every day.
Other ways to help prevent skin cancer include:
- avoiding the strongest sun of the day, between 10 a.m. and 4 p.m.
- encouraging kids to wear wide-brimmed hats and long, loose cotton clothing, especially if they tend to burn easily
- making sure teens understand the dangers of tanning salons
- being a good role model yourself
Not all skin cancer is melanoma, but every case of melanoma is serious. Do what you can to lower your kids’ risk and help them make smart choices about sun safety.
You can find more information online at:
