Psoriasis in children and adults may be confused with eczema, althou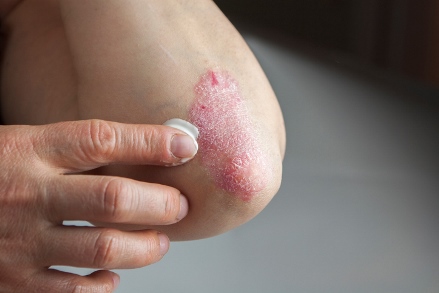 gh it is more commonly mistaken for seborrheic dermatitis. Psoriasis is a skin condition characterized by red, well-demarcated plaques with thick, silvery scale. Psoriasis affects from 1 to 3 percent of Americans, and in about 20 percent of cases, the disease begins before the age of 20 years.
gh it is more commonly mistaken for seborrheic dermatitis. Psoriasis is a skin condition characterized by red, well-demarcated plaques with thick, silvery scale. Psoriasis affects from 1 to 3 percent of Americans, and in about 20 percent of cases, the disease begins before the age of 20 years.
Infantile psoriasis is much less common than atopic dermatitis, and only 2 percent of psoriasis cases present during the first two years of life. There exists a genetic component to this disorder, and multiple family members may be affected. The lesions of psoriasis appear in a usual morphology and distribution pattern. The predominant morphology consists of red, sharply demarcated papules and plaques. It is markedly different than the typical diffuse eczematous lesions of atopic dermatitis. The plaques of psoriasis tend to locate to the scalp, lower back and extremities.
Appearance
In contrast to atopic dermatitis, the extensor surfaces (elbows, knees) are the most commonly affected. Isolated scalp involvement may also be seen in psoriasis, and patients commonly have thick plaques along the frontal hairline. Rarely, psoriasis may present in infants as persistent diaper dermatitis whereas atopic dermatitis does not usually involve the diaper area.
Children with psoriasis tend to have prominent involvement of the eyelids, genital area, and periumbilical area. Some children have a type of disease termed “guttate psoriasis,” with many small, drop-like lesions scattered all over the body of the pediatric patient. Psoriatic lesions are often induced in areas of trauma, the so-called “Koebner phenomenon.”
There are many additional clinical features that, if present, aid in distinguishing psoriasis in children and adults from atopic dermatitis. Psoriasis patients including pediatric psoriasis patients may have nail changes such as onycholysis (separation of the nail plate from the nail bed), yellowing, pitting or delicate nails.
Related Conditions
Psoriatic Arthritis
Approximately 8 percent of psoriasis patients including pediatric psoriasis patients will suffer from psoriatic arthritis. The arthritis may develop prior to the rash, making accurate diagnosis challenging. Psoriatic arthritis is characterized by the involvement of multiple hand and foot joints, most commonly the distal interphalangeal joints. Arthritis may be severe and progress to deformity. Diagnosis of psoriasis is usually made by history and recognition of the typical morphology and distribution pattern. Skin biopsy may be performed in an attempt to clarify the diagnosis in an atypical case.
The following conditions are also associated with psoriasis:
- Obesity
- Heart disease
- Psychological issues
- Inflammatory bowel disease
- Liver disease
Psoriasis Treatment
There are a number of treatments for psoriasis, including topical lubricants, corticosteroids, tar, keratolytics, calcipitriol and tazarotene. The skin condition/disease is often recurrent, and it can be difficult to achieve complete clearing of the rash. Ultra-high potency steroid preparations are often required to manage the thickest plaques. Recalcitrant cases may benefit from psoriasis treatment options, including phototherapy or systemic treatment with retinoids, anti-metabolites, new systemic biologic agents and selective immunomodulatory agents. These psoriasis treatment options require close clinical and laboratory monitoring under the care of a specialist.
Please visit the National Psoriasis Foundation website to learn more: https://www.psoriasis.org