Soiling (Encopresis)
What Is Encopresis?
If your child has bowel movements (BMs) in places other than the toilet, you know how frustrating it can be. Parents might assume that kids who soil their pants are misbehaving or too lazy to use the bathroom when they have the urge to go.
But many kids beyond the age of toilet teaching (generally older than 4 years) who soil their underwear have a condition known as encopresis (en-kah-PREE-sis). They have a problem with their bowels that dulls the normal urge to go to the bathroom. So they can’t control the accidents that usually follow.
Encopresis isn’t a disease. It’s a symptom that may have different causes.
What Are the Signs & Symptoms of Encopresis?
At first, parents may think their child has a simple case of diarrhea. But when it keeps happening, it’s clear that there’s another problem, especially because the child isn’t sick.
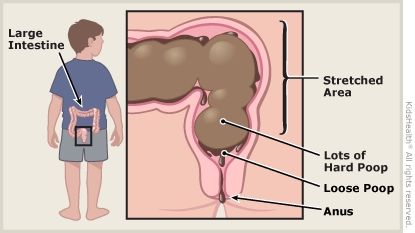
As the buildup of stool stretches the colon, the nerves have trouble telling the brain that it’s time for a BM. If untreated, the soiling will get worse. Then, kids may lose their appetites or complain of stomach pain.
A large, hard poop may also cause a tear in the skin around the anus that will leave blood on the stools, the toilet paper, or in the toilet.
Parents can get frustrated if their child seems unfazed by the poop accidents, which happen mostly during waking hours. Denial may be one reason for a child seeming calm — kids can’t face the shame and guilt they feel about the condition. Some even try to hide their soiled underpants from their parents.
Another reason may be more scientific: Because the brain gets used to the smell of poop, the child may no longer notice the odor.
What Causes Encopresis?
Most encopresis cases are due to constipation. Stool (poop) is hard, dry, and difficult to pass when a person is constipated. Many kids “hold” their BMs to avoid the pain they feel when they go to the bathroom, which sets the stage for having a poop accident.
About Constipation
There’s a wide range when it comes to “normal” pooping. One kid might have one or two BMs per day while another goes only three or four times a week.
A child who passes a soft, medium-sized BM without any problems every 3 days is not constipated. But a child who passes a hard BM (small or large) every other day is. So are other kids who may go every day, but only pass hard little balls and always have poop left behind in the rectum.
Causes of hard poop can include:
- diet
- illness
- not drinking enough liquids
- fear of the toilet during potty training
- limited access to a toilet or a toilet that’s not private (like at school)
Some kids may develop chronic constipation after stressful life events such as a divorce or the death of a close relative.
Rectal surgery or birth defects such as Hirschsprung disease and spina bifida can cause constipation or encopresis without constipation, but this is uncommon.
What Happens With Encopresis?
When a child holds in BMs, the poop starts building up in the rectum and may back up into the colon — and a frustrating cycle begins.
The colon’s job is to remove water from the poop before it’s passed. The longer the poop is stuck there, the more water is removed — and the harder it is to push the large, dry poop out. The large poop also stretches out the colon, weakening the muscles there and affecting the nerves that tell a child when it’s time to go to the bathroom.
Then, the colon can’t easily push the hard poop out, and it’s painful to pass. So the child continues to avoid having a BM, often by dancing, crossing the legs, making faces, or walking on tiptoes.
In time, the rectum and lower part of the colon get so full that it’s hard for the sphincter (the muscular valve that controls the passage of feces out of the anus) to hold the poop in. Partial BMs may pass through, causing the child to soil his or her pants. Softer poop may also leak out around the large mass of feces and stain the child’s underwear when the sphincter relaxes.
Kids can’t prevent this soiling — nor do they have any idea it’s happening — because the nerves aren’t sending the signals that regulate pooping.
How Is Encopresis Diagnosed?
Call the doctor if your child has any of these symptoms of encopresis:
- poop or liquid stool in the underwear when your child isn’t ill
- hard poop or pain when having a BM
- toilet-clogging BM
- belly pain
- loss of appetite
- blood on the toilet paper when wiping or dripping into the toilet bowl
Soiling and constipation are a top reason that kids go to see pediatric gastroenterologists (doctors who diagnose and treat disorders of the stomach and intestines).
How Is Encopresis Treated?
Encopresis is not a behavioral issue or a simple lack of self-control. Punishing or humiliating a child with encopresis will only make matters worse.
Instead, talk to your doctor for help to get through this challenging but treatable problem. The doctor also might recommend that your child see a gastroenterologist.
Treatment happens in three phases:
- Emptying the rectum and colon of the hard poop. Depending on the child’s age and other things, the doctor may recommend medicines, including a stool softener, laxatives, and/or enemas. Give laxatives and enemas only under the supervision of a doctor. Never give these treatments at home without first checking with your doctor.
- Helping your child begin having regular BMs. This is done with the aid of stool-softening agents. It’s important to continue using the stool softeners/laxatives to give the bowels a chance to shrink back to normal size. The muscles of the intestines are stretched out, so they need time to recover.
Parents also will be asked to schedule potty times after meals (when the bowels are naturally stimulated). The child will sit on the toilet for about 5 to 10 minutes. This helps kids learn to pay attention to the urges to go.
- Reducing use of the stool medicines. As regular BMs happen, the doctor will decrease a child’s use of stool softeners and/or laxatives.
Keep in mind that relapses are normal, so don’t get discouraged. Your child might get constipated again or soil their pants during treatment, especially when being weaned off of the stool softeners.
A good way to track your child’s progress is by keeping a daily poop calendar. Make sure to note the frequency, consistency (hard, soft, dry), and size (large, small) of the BMs.
Patience is the key to treating encopresis. It can take several months to a year for the stretched-out colon to return to its normal size and for the nerves in the colon to become effective again.
The Importance of Diet and Exercise
Diet and exercise are very important in keeping stools soft and BMs regular. Make sure your child gets plenty of fiber-rich foods. Serve fresh fruits, dried fruits like prunes and raisins, dried beans, vegetables, and high-fiber bread and cereal.
Try these creative ways to add it to your child’s diet:
- Bake cookies or muffins using whole-wheat flour instead of regular flour. Add raisins, chopped or pureed apples, or prunes to the mix.
- Add bran to baking items such as cookies and muffins, or to meatloaf or burgers, or sprinkled on cereal. (The trick is not to add too much bran or the food will taste like sawdust.)
- Serve apples topped with peanut butter.
- Create tasty treats with peanut butter and whole-wheat crackers.
- Top ice cream, frozen yogurt, or regular yogurt with high-fiber cereal for some added crunch.
- Serve bran waffles topped with fruit.
- Make pancakes with whole-grain pancake mix and top with peaches, apricots, or grapes.
- Top high-fiber cereal with fruit.
- Sneak some raisins or pureed prunes or zucchini into whole-wheat pancakes.
- Add shredded carrots or pureed zucchini to spaghetti sauce or macaroni and cheese.
- Add lentils to soup.
- Make bean burritos with whole-grain soft-taco shells.
Help your child drink plenty of liquids each day, especially water. Diluted 100% fruit juice (like pear, peach, or prune) is an option if your child isn’t drinking enough water. Also, limiting your child’s daily dairy intake (including milk, cheese, and yogurt) may help.
What Else Should I Know?
Successful treatment of encopresis depends on the support a child gets. Some parents find that positive reinforcement helps to encourage the child throughout treatment. For instance, put a star or sticker on the poop calendar for having a BM (or even for trying to), sitting on the toilet, or taking medicines.
Don’t blame or yell — it will only make your child feel bad and it won’t help manage the condition. With lots of love, support, and reassurance that they’re not the only one in the world with this problem, your child can overcome encopresis.
