Hydrocephalus
What Is Hydrocephalus?
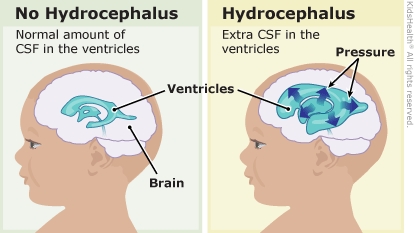
Hydrocephalus is a buildup of cerebrospinal fluid (CSF) in the hollow places inside the brain. These hollow places are called ventricles. The buildup of CSF can put pressure on the brain.
Treatments for hydrocephalus (hi-droh-SEF-eh-less) usually can lower the amount of CSF.
What Are the Signs & Symptoms of Hydrocephalus?
Signs and symptoms of hydrocephalus in babies and children can include:
- fussiness
- tiredness
- poor appetite
- vomiting
- eyes that stay looking down
- slowed development
Babies younger than 1 year old still have their “soft spot” because their skull bones have not fully grown together yet. In them, hydrocephalus usually leads to bulging at the soft spot, increasing head size, and large scalp veins.
Older children with hydrocephalus usually complain of headache.
Who Gets Hydrocephalus?
A child can:
- be born with hydrocephalus (called congenital hydrocephalus)
- get it later (called acquired hydrocephalus)
Hydrocephalus can run in families.
How Does Hydrocephalus Happen?
Cerebrospinal fluid is saltwater that’s made inside the ventricles. It flows around the brain and spinal cord, cushioning them. It also sends nutrients to the brain and takes away waste. Then it’s absorbed into the bloodstream, and new, fresh CSF takes its place.
Hydrocephalus can happen if:
- The flow of CSF is blocked (called obstructive hydrocephalus).
- Not enough CSF is absorbed into the bloodstream (called communicating hydrocephalus).
What Causes Hydrocephalus?
Causes of hydrocephalus include:
- spina bifida: when a baby’s spinal cord does not fully develop
- aqueductal stenosis: when CSF flow between the ventricles inside the brain is blocked
- infection during pregnancy
- complications of prematurity (being born early)
- bleeding in the brain (from a stroke or brain injury)
- a brain tumor
- infection in the brain
How Is Hydrocephalus Diagnosed?
Doctors diagnose hydrocephalus by:
- asking about symptoms
- doing an exam
- doing imaging studies such as an ultrasound, CT scan, or MRI
How Is Hydrocephalus Treated?
Treatment for hydrocephalus depends on the child’s age and what’s causing the hydrocephalus.
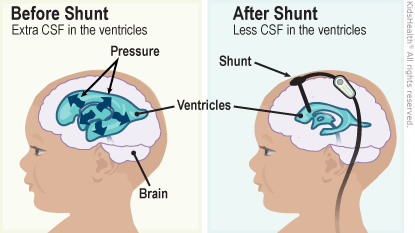
Treatments may include one of these surgeries:
- Ventriculoperitoneal (VP) shunt surgery: Doctors place a tube from the brain’s ventricles to the peritoneal cavity, the space inside the belly where the stomach and the bowels sit. The tube is all inside the body under the skin. After it gets to the belly, the extra CSF is absorbed into the bloodstream. Shunts are replaced:
- over time as a child grows and needs a bigger shunt
- if they get infected or stop working
- Endoscopic third ventriculostomy (ETV) surgery: A tiny hole made in the bottom of the ventricle lets the extra CSF drain out of the brain. Then, it’s absorbed into the bloodstream.
Kids also might need therapy for slowed development, such as:
- an early intervention program
- physical therapy
- occupational therapy
How Can Parents Help?
Your child needs your care and support. Treatment for hydrocephalus is successful in many children. But most need more than one surgery and ongoing medical care.
To help your child get the best treatment:
- Take your child to all doctor visits.
- Follow all medical recommendations, such as taking prescribed medicines.
- If needed, take your child to:
- early intervention programs
- physical therapy
- occupational therapy
