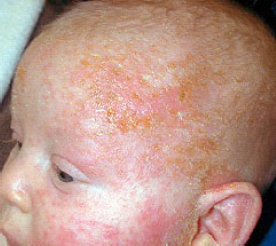
This infant has atopic dermatitis, characterized by itchy, red, often oozing patches on the cheeks. The rash was successfully treated with prescription cortisone ointment & moisturizers.
Eczema: What is it?
Eczema refers to a number of skin conditions, all of which possess red itchy lesions. Seborrheic dermatitis, contact dermatitis, nummular eczema, and atopic dermatitis can all present with red itchy eczema patches. The most common cause of eczema in childhood is atopic dermatitis. The following discussion relates to this disorder.
How common is it?
Approximately 15 percent of children have eczema. Many children improve with age, and patients may clear completely before adolescence. This disease clearly runs in families, and if both parents have eczema, the risk of a child approaches 50 percent.
What causes it?
Although the exact cause is unknown, a clear relationship exists between atopic dermatitis and other types of hypersensitivity to the environment, such as asthma, and hay fever. Thirty to 50 percent of children with atopic dermatitis will eventually develop either asthma or hay fever, and it is quite common to have other relatives with these conditions. It is not possible to “catch” atopic dermatitis. He/she was born with the tendency to have it.
What does it look like?
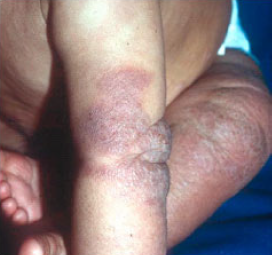
Atopic dermatitis usually begins in infancy, after 2 months of age, but it can start later. The skin is dry and the rash is quite itchy, so infants may be restless and rub against the sheets, or scratch if able. The rash may involve the face and it may cover a large part of the body. As the child gets older, the rash may become more localized. In early childhood, the rash is commonly on the legs, feet, hands and arms. As a person becomes older, the rash may be limited to the bend of the elbows and knees, on the back of the hands, feet, and on the neck and face. As the rash becomes more established, the dry itchy skin may become thickened, leathery and sometimes darker in color.
The more the person scratches, the worse the rash is and the thicker the skin gets. The skin is easily irritated by sweating, environmental changes, wool clothing, playing on the grass, too much soap, excessive swimming, etc. Scratching may then lead to secondary bacterial infection at the sites where the skin is damaged. Most children with atopic dermatitis outgrow the condition before school age; some continue to have problems as an adolescent or even as an adult.
Do foods cause it?
The majority of children with atopic dermatitis do not have identifiable allergies to foods, and the ones who do often show little improvement when that food is avoided, thus for the majority of patients with atopic dermatitis, extensive evaluations for such allergies are unproductive. In a small group of atopics, however, significant food sensitivities can be documented. The foods most likely to aggravate atopic dermatitis include milk, eggs, nuts, soy, wheat, and seafood. In patients with severe or refractory eczema, evaluations for such allergies may be appropriate.
How is it treated?
There is no magic cure for atopic dermatitis. In fact, there is no cure at all. However, in most cases we can have considerable success, if treatments are maintained. The following are treatment recommendations for the child with eczema:
- Moisturize the skin frequently and avoid irritation! Moisturizers help protect the skin thus making it better able to act as a barrier against things that irritate it. Although topical prescription products may improve a child’s condition, the patient will not remain clear once the steroids are discontinued unless moisturizers are routinely used. Determining the best moisturizer for any one patient is frequently a trial and error process, as some patients may be sensitive to a product that works fine for the majority of patients. Moisturizers should be used EVERYDAY. Try to keep as much natural skin oil as possible by minimizing bathing and soap.
- Minimize scratching! Scratching leads to a break in the skin barrier, risking possible infection, and makes the rash worse. Keep nails trimmed and smooth. Use antihistamines when itching occurs, and remember that the dose of antihistamines may need to be increased to be effective. In contrast, if your child’s dose causes significant daytime drowsiness, decrease the dose. Occasionally children will become over-excited by antihistamines. Notify your doctor if this occurs.
- Do not be afraid to use topical steroids, but do not over-use them either! Over-use can lead to damage of the skin (thinning, easy bruising, and development of small blood vessels), or over-absorption into the body and interference with growth. These side effects are exceedingly unlikely if steroid ointments are used as directed. There are many strengths and types of topical steroid creams and ointments. The lowest strength necessary to control the eczema should be used. Topical steroids are important and quite useful treatments. They must be used as directed by the physician. Ointments should be used instead of creams whenever possible.