The importance of sagittal plane alignment in treating spinal disorders is widely recognized. However, much of our current understanding of sagittal alignment is derived from studies of patients with disease, degenerative change, or known deformity, when the goal is a normal prole.
Recent research led by Michael P. Kelly, MD, MSc, at Rady Children’s Hospital-San Diego, in the journal Spine sheds new light on measures of sagittal alignment that may better inform surgical decision-making. Additionally, Dr. Kelly aims to bring this knowledge from the adult population to the pediatric patients at Rady Children’s.
For example, the study identied the C2 tilt angle as a reliable measure of global sagittal balance, while the L1 pelvic angle may be a superior measure of spinopelvic alignment compared to what is currently being used. Additionally, the T4 pelvic angle has been shown to correlate closely with the L1 pelvic angle. These newer measures hold promise as potential alignment targets that are directly modiable in surgery.
While previous alignment targets have utilized postural measures that are not directly modiable in surgery, newer measures such as the vertebral pelvic angles may hold promise as potential alignment targets. Sagittal alignment targets should aim to restore patients to a normal global balance using parameters that are easily measured and directly modiable in surgery and conditioned on adjacent regional alignment. By defining normal global sagittal balance using parameters that are directly modiable in surgery and conditioned on adjacent regional alignment, physicians can better restore patients to a normal alignment.
Study Design and Participants
To define normal global sagittal balance, the study recruited healthy volunteers over 18 years of age with no history of spinal disease or surgery. Individuals who met the inclusion criteria (320 out of 485 volunteers) were enrolled and examined for the relationship between sagittal balance, spinopelvic alignment, lordosis, and global sagittal balance. The median age was 37 and 61% were female.
The researchers used specialized software to measure various spinal and pelvic angles from low-dose stereoradiographs. Patient characteristics and alignment measures were reported using median values and frequency proportions. They used statistical models to assess associations between pelvic tilt and vertebral body tilt at different spinal levels and determined correlation with pelvic incidence using Spearman’s rank correlation. Linear regression models were used to estimate normal sagittal Cobb angles for each vertebra and vertebral pelvic angles by pelvic incidence alone.
A Strong Connection Revealed
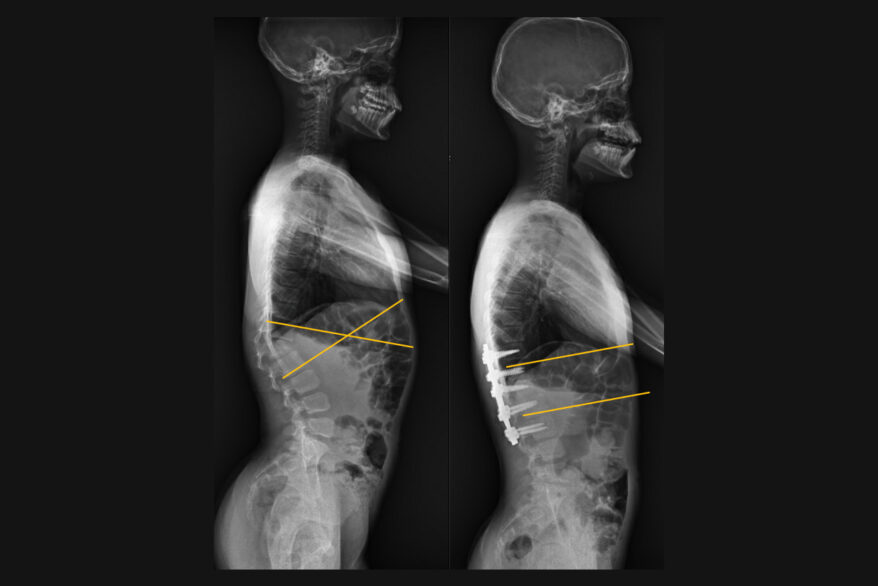
The study revealed strong connections between pelvic tilt and C2, T4, and L1 pelvic angles, with vertebral tilt narrowing in more cranial levels. While pelvic tilt was moderately correlated with pelvic incidence, vertebral tilt from C2 to L4 was not. Predicting the sagittal Cobb angle (lordosis) by pelvic incidence alone resulted in low explained variance, but L4-S1 lordosis was independent of pelvic incidence. Pelvic incidence had a significant association with all vertebral pelvic angles, especially in more caudal levels. Valuable Insights Gleaned for Better Surgical Outcomes An equation was established to describe a normal L1 pelvic angle relative to pelvic incidence. This measure is superior to the commonly used lumbar lordosis, as the L1 pelvic angle accounts for both the magnitude of lumbar lordosis and the shape of the lordosis. As pelvic incidence increased, L1 pelvic angle and L1-S1 lordosis also increased. Radiographs of volunteers with high and low pelvic incidence indicated that despite extreme values, the C2 tilt was within 1° and the difference in T4 and L1 pelvic angles was less than 1°. This indicates some commonalities in sagittal alignment across a population.
The findings highlight the significance of considering various factors like pelvic incidence, L1 pelvic angle, and lumbar lordosis when prescribing sagittal balance and spinopelvic alignment for better patient outcomes. The study also provides valuable insights into the relationship between these factors in individuals with varying pelvic incidences. By utilizing newer measures and targets that are directly modiable in surgery, we hope to improve overall quality of life and provide better outcomes for both adult and pediatric patients.
To learn more about the top-ranked Orthopedics program at Rady Children’s, click here.