Doctors use a number of pieces of information to help diagnose a patient with atopic dermatitis. These include but are not limited to the following:
Past Medical History
It is important for doctors to know as much about your child’s personal medical history as possible because many cases of atopic dermatitis present as patterns that are similar (or, at least, close to the same) from one patient to the next.
For example, more than half of all atopic dermatitis begins during the first 12 months of life (most commonly between 3 and 6 months of life), and most atopic dermatitis begins in the first 10 years of life. Because of this fact, physicians can use the age at which a child’s rash first appeared to help confirm the diagnosis of atopic dermatitis. In other words, the fact that an itchy rash first appears in a patient at 22 years of age makes atopic dermatitis possible but less likely.
Children with atopic dermatitis may also have a history of other disorders such as allergies/hay fever and/or asthma that may aid in establishing a diagnosis. This is because allergies/hay fever and asthma are known to be associated with atopic dermatitis. Together, these three conditions are known as “the atopic triad.” The likelihood of developing atopy increases with age. This progression from one condition to the other is referred to as the atopic march.
Physical Examination
The rash of atopic dermatitis typically exists as three age-related phases, with each phase having its own location of involvement and appearance. It is important to know that these stages may overlap with one another. The three phases are as follows:
Infantile Phase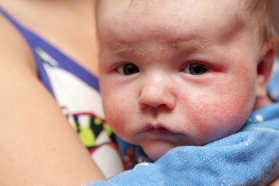
Infantile atopic dermatitis occurs, typically, from about 2 to 3 months of age to about 2 to 3 years of age. It often appears, first, on the cheeks and scalp. The wrists, legs, arms, neck and areas around the ears are also commonly involved. Chest and back involvement is common, but the diaper area is usually spared, probably because the skin in this area remains moist.
In general, the rash of this infantile phase tends to show up fairly suddenly on both sides of the body as scaly, red patches. Weeping and crusting may also be present in severe cases. Generalized dry skin can help to make the diagnosis. Chronic changes (i.e., those that occur over time with long-standing disease) like thickening of the skin are not a common feature in the infantile phase.
All affected infants experience itching (pruritus), one of the hallmarks of atopic dermatitis. The itch-scratch-itch cycle can develop as early as three months of age. Infants may rub against objects such as carpet or bedding as a substitute for direct scratching. Itching is a major cause of other problems in atopic dermatitis and often leads to poor sleep and/or skin infections. Itching can be quite intense and is often a source of extreme frustration for parents.
Childhood Phase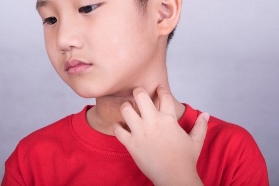
During the childhood phase, which appears from about 2 years of age to puberty, the rash of atopic dermatitis begins to resemble that seen in the adult phase. More specifically, the elbow and knee creases are the major sites of involvement. Other frequently involved sites include the neck, wrists, ankles, and the creases between the thighs and buttocks.
As in the infantile phase, this rash tends to be poorly-defined, scaly, red patches with or without crusting and scratches. Thickening of the skin becomes a very noticeable feature during the childhood phase and tends to be most evident at the wrists and ankles. The skin may also commonly appear bumpy, resembling “goose bumps” (perifollicular accentuation); this is especially true in darker skinned children with atopic dermatitis.
Patients often have lightening (hypopigmentation) or darkening (hyperpigmentation) of the skin in areas where they previously had eczematous rash. These color changes often cause concern among parents who worry the color changes will be permanent. In general, the rash of atopic dermatitis does not scar unless (1) the skin gets severely infected or (2) the skin is severely damaged from repeated scratching. Normal color generally returns weeks to months after the active eczematous rash resolves.
Adulthood Phase
After puberty, the rash of atopic dermatitis continues to involve the creases of the arms and legs and can be at one or more sites, covering much of the body’s skin.
Additionally, long-standing “hand and foot” dermatitis may become a noticeable feature in teenagers and adults and may be the only sign of atopic dermatitis for some patients. Neck and facial involvement also tend to be more noticeable than in the childhood phase, and some patients have severe disease around the eye.
Adults tend to have more scaling and less crusting than infants and children. In general, older patients have more long-term findings than younger patients; as such, dry skin and skin thickening are common features that aid in diagnosis. Skin darkening (hyperpigmentation) or lightening (hypopigmentation) is also common.
Family History
A family’s medical history is often helpful in establishing a diagnosis of atopic dermatitis. Because it has long been recognized that atopic dermatitis, allergies/hay fever and/or asthma (together known as the atopic triad) run in families, doctors can use the fact that other family members have suffered from one or more of these conditions to help confirm the diagnosis of eczema in a new patient.
In 1916, a classic study showed that children with one allergic parent develop allergy 50 percent of the time, increasing to 75 percent if both parents were allergic. Many subsequent studies have confirmed this data. Overall, about 70 percent of atopic dermatitis patients will have a family history of atopy.
Consequently, parents should share with the doctor any family history of asthma, allergies/hay fever or atopic dermatitis. Absence of an atopic family history makes the diagnosis of atopic dermatitis in a new patient still possible but less likely.